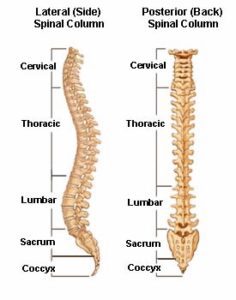
About Spinal Conditions
The different types of spinal conditions are:
For more information, please visit www.spineuniverse.com
Spinal Conditions
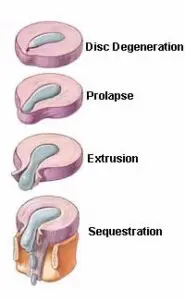
A slipped disc can happen anywhere in the spine and does not actually slip. Instead, the disc, located between the spine’s bones (vertebrae), splits or ruptures. When this happens, the inner gel-like substance (nucleus pulposus) leaks out. This is called a herniation of the nucleus pulposus—or a herniated disc. People between the ages of 30 and 50 are most at risk for herniation because the elasticity and water content of the nucleus pulposus decrease with age.
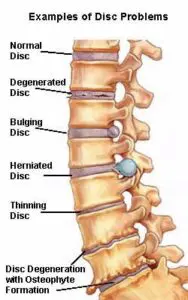
SYMPTOMS:
Symptoms of a herniated disc may include dull or sharp pain, muscle spasm or cramping, weakness, tingling, or referred pain.
CAUSES OF HERNIATED DISC:
Pain from a herniated disc is often the result of daily wear and tear on the spine. However, it may also be caused by an injury.
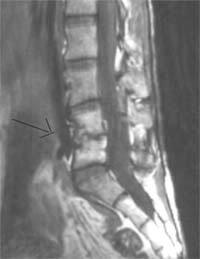
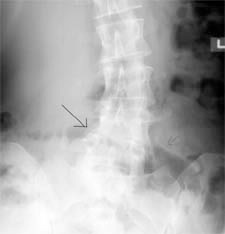
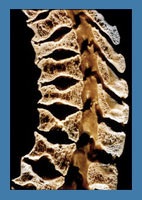
Discitis, or disc space infection, is an inflammatory lesion of the intervertebral disc that occurs in adults but is more commonly in children. Its cause has been debated, although most authors believe it is infectious. The infection probably begins in one of the continuous end plates, and the disc is infected secondarily. Severe back pain that begins insidiously is characteristic of the disease. They rarely have an elevated temperature, and their white blood cell count is frequently normal. However, the erythrocyte sedimentation rate is usually increased.
Lateral radiographs of the spine usually reveal disc space narrowing with erosion of the vertebral end plates of the contiguous vertebrae. Bone scanning may help localize a lesion that is difficult to diagnose clinically. Some bone scans are falsely negative, so the diagnosis of disc space infection should not be excluded simply because the bone scan is normal. Magnetic resonance imaging (MRI) seems to help identify a disc space infection. The appropriate treatment of these lesions has been the subject of controversy.
Visit our site at www.spinefracture.org to learn more.
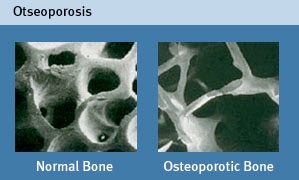
Osteoporosis
Osteoporosis is a systemic skeletal disease characterized by reduced bone mass and deterioration of bone tissue architecture. This results in bone fragility and susceptibility to fractures.
Osteoporosis affects 100 million people worldwide, and 28 million people in the United States are at risk. Each year, there are 1.5 million fragility fractures in the United States. Of these, 700,000 occur in the spine, 300,000 in the hip, 250,000 in wrists, and 250,000 in other bones. According to the National Osteoporosis Foundation, the projected cost of treatment of this disease in the United States in 2030 is $60 billion.
Vertebral Compression Fractures
Prevalence
Spinal vertebral compression fractures are the most common fracture due to osteoporosis. In the United States, there are 700,000 compression fractures yearly, or one compression fractures every 45 seconds! A quarter million patients with their first painful fracture are diagnosed each year. After patients suffer one compression fracture, the risk increases for subsequent fractures 5-fold.
Acute Signs and Symptoms
Vertebral compression fractures present with the sudden onset of back pain with little or no trauma. It may be the first sign of osteoporosis. The vertebra collapses, and the spine shortens and tilts forward. Like any bone fracture, it hurts.
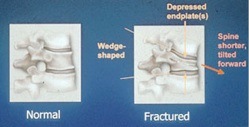
Chronic Signs and Symptoms
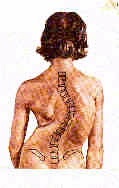
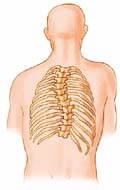
When osteoporosis is left untreated, multiple spinal compression fractures may occur over time. Patients experience episodic and recurrent back pain. Multiple fractures cause collapse and a forward tilt of the spinal column, as depicted in the skeleton below.
Scoliosis is a medical term taken from a Greek word meaning curvature. This disease is known to develop in adults over 18, causing the spine to curve laterally (to the side) to the left or right. Adult scoliosis is caused by:
- Progression of the disease from childhood. This usually occurs when scoliosis is not treated early or goes unnoticed during childhood. The scoliotic curves may be thoracic, lumbar, or both.
- The asymmetric degeneration of spinal elements. This may be caused by osteoporosis (porous bone), disc degeneration, compression fracture, or a combination. These conditions usually affect the lumbar spine and can affect vertebral height, shape, or structural integrity.
FACTS AND TIPS FOR SCOLIOSIS
SYMPTOMS OF SCOLIOSIS:
A spinal cord injury (SCI) involves damage to the spinal cord and nerve roots. Car accidents, falls, violent acts, and non-traumatic disorders can injure the spinal cord. SCI temporarily or permanently stops or alters the ability of the brain to communicate with other parts of the body.
Diagnosis
When spinal cord injury is suspected (e.g., spinal fracture), immediate medical attention is required. Spinal cord injury (SCI) is usually first diagnosed when the patient presents with a loss of function below the level of injury.
The initial evaluation includes x-rays, a CT scan, and possibly an MRI. Fractures are demonstrated on plain radiographs. CT scanning and MRI studies are used to evaluate the soft tissues in the spinal column. In addition, a myelogram may be performed to identify and evaluate spinal cord lesions caused by trauma or disease.
CAUSES OF SPINAL CORD INJURY
The most common traumatic SCI causes include:
Signs and Symptoms of Possible Spinal Cord Injury
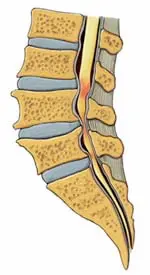
Spinal Stenosis is the narrowing of your spine. In a more detailed explanation, spinal stenosis is when the channels your spinal cord and nerve roots travel through become narrower-so narrow that your spinal cord and nerve roots get squeezed. Doctors often call this squeezing "compression."
Since spinal stenosis can gradually develop as you age, the symptoms can also gradually develop—and gradually get worse. Also, symptoms can vary a great deal. You may have no symptoms since narrowing the spinal canal, or other channels, does not always compress the spinal cord or nerves. But when your spinal cord or nerve roots become compressed and squeezed, you'll feel it.
Your symptoms also depend on where your spinal canal has narrowed. Generally, spinal stenosis affects your low back (lumbar spine) or your neck (cervical spine). It's not as common to have stenosis in your mid-back (thoracic spine).
FACTS AND TIPS ABOUT SPINAL STENOSIS:
Many years ago, spinal stenosis was called "creeping paralysis" because it gradually worsens as you age. Most people thought that once it started, there wasn't much you could do to stop spinal stenosis. Along with forgetfulness, the pain from spinal stenosis was assumed to be just another part of growing old.
The risk of developing spinal stenosis increases in those over 50.
Spinal tumors rarely occur and are either benign or malignant. Some tumors are known to metastasize (spread) via arteries, veins, the lymphatic system, and directly. Malignant tumors of the breast, prostate, lung, and kidney can spread into the spine. Spinal tumors can be dangerous when they cause spinal canal compression, which may lead to neurologic dysfunction (e.g., paralysis).
Symptoms of Spinal Tumors
The primary symptom of a spinal tumor, which brings most patients to seek medical advice, is non-mechanical back pain. Non-mechanical back pain is different from the more common mechanical back pain. Mechanical back pain due to muscle strains or disc injury usually worsens with activities such as sitting, bending, and walking and gets better with rest or lying down, whereas non-mechanical back pain is constant and is not improved by rest or lying down. Other symptoms include:
Symptoms of spinal tumors generally develop slowly and worsen over time unless they are treated.
CAUSES OF SPINAL TUMORS:
Spinal tumors, whether they're primary or secondary tumors, are caused by abnormal cell growth.
In primary spinal tumors (tumors originating in the spine), researchers aren't sure what causes the cells to grow abnormally. In some cases, it may be related to radiation exposure or chemicals that cause cancer; it's possible that the environment plays a role. Genetics may also play a role: for example, neurofibromatosis is a hereditary disorder that involves tumors on or near the spinal nerves.
For most cases of primary spinal tumors, though, the medical community isn't sure what causes primary tumors.
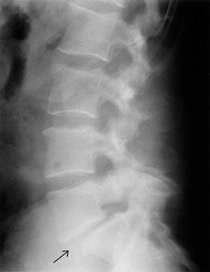
Spondylolisthesis is when one vertebra slips forward over the vertebra below it. Most often, that happens in the low back (lumbar spine) because that part of your spine bears much weight and absorbs a lot of directional pressure. In other words, your lumbar spine has to move quite a bit (rotate in various directions) while carrying your body weight. Sometimes, this combination can put so much stress on the vertebrae that one of them slips forward.
The x-ray below gives you a good example of spondylolisthesis. Look at the area the arrow points to, you can see that the vertebra above the arrow isn't in line with the vertebra below it. It's slipped forward; it's spondylolisthesis.
SYMPTOMS OF SPONDYLOLISTHESIS:
Many people with spondylolisthesis are symptom-free. Sometimes, a spondylolisthesis is discovered when the patient has an x-ray for an unrelated problem. However, some patients do have symptoms that range from mild to severe.
Listed below are several symptoms usually related to spondylolisthesis:
Low back pain and tenderness
Spondylolisthesis can be caused by: